
In summary:
- Briefing your partner is not about giving tasks, but transferring responsibility to make them a confident advocate.
- Focus on practical skills like counter-pressure and specific communication for the intense transition phase.
- Proactively plan for unexpected scenarios, like an emergency C-section, by creating a “Plan B” together.
- Address the mental load imbalance early by teaching advocacy as a shared skill, not just a list of duties.
The question echoes in the minds of so many expectant mothers: “What if, when I need them most, my partner just freezes?” You’ve likely read the advice: pack a hospital bag for them, tell them to offer you water, maybe even show them a massage technique. These are helpful tasks, but they don’t address the core fear—the fear that in the heat of the moment, the full weight of decision-making, of advocating, of remembering every preference, will fall right back onto your shoulders.
The common approach is to create a list of duties. But what if the true key to a supportive partnership in labour isn’t in delegating tasks, but in systematically transferring responsibility? What if you could transform your loving, but potentially overwhelmed, partner from a worried bystander into an empowered co-pilot, fully equipped to navigate the journey alongside you? This isn’t just about what they should *do*, but about what they need to *know* to act with confidence and be your voice when you are busy with the powerful work of birth.
This guide moves beyond simple to-do lists. We will explore how to have strategic conversations, how to practice tangible skills, and how to plan for the unexpected. Together, you will build a toolkit that empowers your partner to be the advocate you both deserve, shifting the dynamic from one of delegation to one of true, resilient partnership.
To help you build this powerful partnership, this article breaks down the essential skills and mindset shifts needed. The following sections will guide you through practical techniques, communication strategies, and planning for every eventuality, ensuring your partner is ready to be your rock.
Summary: How to Turn Your Partner Into an Empowered Advocate for Labour
- What Should Your Partner Do During Transition When You Are Beyond Words?
- How Can Your Partner Use Counter-Pressure to Reduce Back Labour Pain by 50%?
- What Your Partner Needs in Their Own Hospital Bag for a 36-Hour Labour?
- Why Sitting Silently on Your Phone Leaves Your Partner Feeling Abandoned in Labour?
- How to Prepare Your Partner for the Possibility of an Emergency C-Section Decision?
- How to Write a Plan B for Emergency C-Section So You Still Feel in Control?
- Why “Just Tell Me What to Do” Still Leaves All the Planning With You?
- Why Mothers Still Carry 71% of the Mental Load Even With “Hands-On” Partners?
What Should Your Partner Do During Transition When You Are Beyond Words?
The transition phase of labour is often the most intense and primal. It’s the point where you might feel you “can’t do this anymore,” and verbal communication becomes difficult, if not impossible. This is the moment your partner’s preparation truly shines. Their role shifts from conversational support to being a grounding, reassuring presence. Instead of asking questions, they should offer simple, powerful mantras. Short, repeated phrases like “I’m here,” “You are safe,” or “Breathe with me” can become an anchor in the storm of sensations. The goal is not to distract you, but to help you stay centred.
It’s vital for partners to understand that the intensity of transition is a sign of progress, not a crisis. Seeing you in this powerful state can be overwhelming if they expect the dramatised scenes from movies. As veteran doula Melissa Cowl notes, real birth is often quieter and more focused. In her experience, “In 15 years of attending births as a doula, I have never seen women behave the way they do in movies, screaming and hitting their partners.” Your partner’s calm presence, perhaps just breathing in sync with you or providing steady physical contact, can be the most profound support they offer. They should learn to recognise the signs of transition as a positive milestone—a signal that you are very, very close to meeting your baby.
This is where pre-labour conversations are crucial. You can practice which phrases feel most supportive to you. Some people prefer encouragement (“You are so strong”), while others need practical reminders (“Soften your jaw”). By discussing this beforehand, your partner has a clear, simple job to do when you are beyond words, allowing them to feel effective and connected rather than helpless. Their quiet confidence becomes a source of strength for you.
How Can Your Partner Use Counter-Pressure to Reduce Back Labour Pain by 50%?
For many women experiencing “back labour,” often caused by the baby’s position, the pain can feel concentrated and overwhelming. This is a key moment where a partner can move from being a spectator to a hands-on hero. Counter-pressure is a simple but profoundly effective technique that can provide significant relief. It involves applying firm, steady pressure to the lower back to counteract the internal pressure from the baby’s head. This is a tangible, learnable skill that empowers your partner to actively reduce your pain.
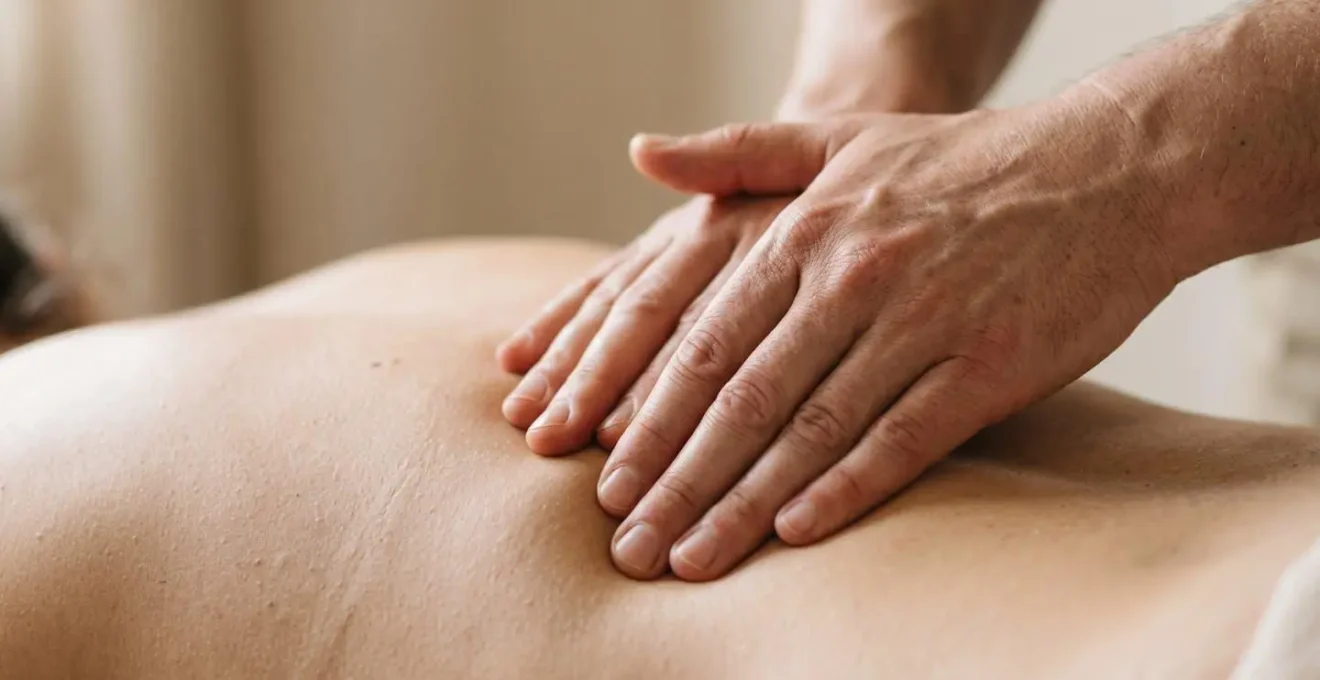
As the illustration shows, the most common and effective technique is sacral counter-pressure. Here’s how your partner can practice and apply it:
- Find the Spot: Between contractions, ask your partner to place the heel of their hand or their knuckles on your sacrum—the triangular bone at the base of your spine. You will guide them to the exact point that feels most relieving.
- Apply Steady Pressure: They should lean in with their body weight, not just push with their arms, to apply firm, consistent pressure throughout the contraction.
- Communicate and Adjust: The right amount of pressure is key. Your partner can watch your breathing and listen to your sounds to gauge effectiveness, asking for feedback like “more pressure?” or “is that the spot?” between contractions.
- Explore Other Techniques: Besides sacral pressure, the double hip squeeze (squeezing the hips together) can also open the pelvis and relieve pain, especially if the baby is in a posterior position.
Practicing these techniques before labour begins is invaluable. It builds muscle memory for your partner and allows you to provide feedback in a calm environment. This isn’t just a massage; it’s a therapeutic intervention. By learning this skill, your partner gains a concrete tool to support you, transforming their feelings of helplessness into a sense of purpose and direct contribution to your comfort.
What Your Partner Needs in Their Own Hospital Bag for a 36-Hour Labour?
While most of the focus is on the mother’s and baby’s hospital bags, preparing a “go bag” for the birth partner is a critical step in planning for endurance. Labour can be a marathon, sometimes lasting 24, 36, or even more hours. A partner who is hungry, dehydrated, or uncomfortable cannot provide their best support. Packing their own bag is an act of foresight that ensures they can stay by your side, focused and energized, without needing to leave for supplies. This isn’t selfish; it’s a core part of the “empowered co-pilot” role.
The partner’s bag should focus on endurance, comfort, and practical support tools. Think of it as a long-haul flight kit. Key items include:
- Fuel and Hydration: A reusable water bottle and a variety of snacks are non-negotiable. Pack a mix of quick-energy foods (like granola bars) and more substantial, protein-rich options (like nuts or jerky) to avoid reliance on hospital cafeterias with limited hours.
- Tech Essentials: A fully charged phone is a given, but a high-capacity power bank (at least 20,000 mAh) and an extra-long charging cable (10 feet/3 metres) are the real game-changers, allowing them to stay connected without being tethered to a wall socket far from you.
- Personal Comfort: A change of comfortable clothes, a toothbrush, deodorant, and any personal toiletries will make a world of difference during an overnight stay. They will feel more human and better able to support you.
- Your “Briefing” Tools: A laminated copy of the birth plan with key advocacy phrases highlighted for quick reference during intense moments.
This preparation should be done well in advance. In fact, maternal health experts suggest partners should have their hospital bag packed by 32 to 36 weeks gestation. By taking responsibility for their own needs, partners are not just caring for themselves; they are ensuring they have the physical and mental stamina to be the unwavering support system you need, for as long as you need it.
Why Sitting Silently on Your Phone Leaves Your Partner Feeling Abandoned in Labour?
In a world where phones are our constant companions, it’s natural to reach for one during moments of quiet or uncertainty. However, in the labour room, a partner silently scrolling on their phone can send a powerful and often painful message: “I am not here with you.” Even if they are just looking up information or passing time during a lull, the act of gazing into a screen creates a digital wall. It breaks the intimate connection of the shared experience and can make the labouring person feel profoundly alone and unsupported at a time when they are at their most vulnerable.
The feeling of abandonment is not about the partner’s intent, but about the impact of their action. To the labouring mother, who is fully immersed in a powerful physical and emotional process, seeing her partner disengaged—even for a moment—can be jarring. It can feel like they have checked out, leaving her to face the intensity alone. This is also a moment where a partner may miss subtle cues for support, like a shift in breathing or a need for a sip of water, because their attention is divided.
This doesn’t mean phones must be banned entirely. The key is to transform the phone from a distraction into a collaborative tool. Discuss and agree on “permitted phone use” beforehand. A phone can be an incredible asset when used intentionally for support:
- As a Timer: Using a contraction timer app is an active, helpful task, providing valuable data for you and the medical team.
- As a DJ: Playing the pre-agreed labour playlist or calming sounds to manage the atmosphere.
- As a Researcher: Quickly looking up a medical term the doctor just used to help you both understand what’s happening.
- As a Communicator: Sending a pre-written update to a single designated family contact to manage the flow of information outwards.
A simple guideline to establish is the “One-Hand Rule”: if they need to use the phone, the other hand should maintain physical contact with you—holding your hand, resting on your shoulder. This small action maintains the physical and emotional connection, ensuring the phone is a tool within the partnership, not a barrier between you.
How to Prepare Your Partner for the Possibility of an Emergency C-Section Decision?
The moment a vaginal birth plan shifts to an emergency caesarean section can be fast-paced, clinical, and emotionally charged. For a birthing person, it can feel like a loss of control. For a partner, it can trigger fear and uncertainty, making it the ultimate test of their advocacy skills. This is precisely the scenario where a pre-briefed partner is most valuable. Their role is to remain calm, act as your ears and advocate, and help you process information when you may be overwhelmed or exhausted.

Preparing for this possibility is not about manifesting a negative outcome; it’s about ensuring you have a safety net of support, no matter what turn your birth takes. The goal is for your partner to be a stable presence, helping to maintain a sense of dignity and informed consent throughout the process. Their preparation allows them to filter the urgency and focus on what you need to know and feel. It is vital they are ready to step into this role with clarity and confidence, which is achieved by discussing the plan and their role in detail beforehand.
Your Partner’s Advocacy Checklist for an Emergency Situation:
- Assess the Urgency: The first action is to ask the critical time question: “Is the baby or mother in immediate danger right now, or do we have a few minutes to discuss this?” This simple question helps frame the situation and determines the pace of decision-making.
- Gather Key Information: Their role is to listen intently to the medical team’s reasoning. They should be prepared to ask clarifying questions like, “Can you explain what that means for us?” to ensure both of you understand the ‘why’ behind the decision.
- Confirm Your Consent & Dignity: The partner’s job is to be your voice. They should ensure you are being spoken to directly and that your consent is being given. They can say, “I need to make sure my partner understands what is happening. Can you explain it to her one more time?”
- Advocate for ‘Plan B’ Preferences: This is where your pre-written ‘Plan B’ comes in. The partner’s role is to remember and request your gentle C-section preferences, such as asking for the drape to be lowered or ensuring skin-to-skin is attempted in the operating room.
- Provide Narrative Support: If you are separated from the baby, or if things are moving quickly, the partner becomes the narrator. Their job is to stay with you or the baby and provide a calm, reassuring account of what is happening to bridge any gaps in your experience.
How to Write a Plan B for Emergency C-Section So You Still Feel in Control?
The term “birth plan” can sometimes feel fragile, easily shattered by the unpredictability of labour. That’s why creating a “Plan B” or a set of “birth preferences for an unexpected caesarean” is one of the most empowering actions you can take. It’s an acknowledgement that while you cannot control every aspect of birth, you can still have preferences and advocate for an experience that is respectful, gentle, and family-centred, even in an operating room. This document becomes your partner’s script, giving them concrete points to advocate for when things are moving fast.
This is not a list of demands, but a conversation starter with your medical team and a guide for your partner. The goal is to bring elements of a physiological birth into a surgical setting, focusing on connection and sensory experience. Discussing and writing these preferences down together is a powerful bonding exercise. It ensures your partner knows what is most important to you, allowing them to focus their advocacy efforts effectively. This proactive planning helps transform a potentially frightening experience into one where you still feel seen, heard, and in control of what can be controlled.
Your “Plan B” can be a simple, one-page document. Here are some key preferences you might want to discuss and include, often referred to as a “Gentle Cesarean Preference Checklist”:
- Sensory Environment: You can request that your chosen playlist be played in the operating room, that voices are kept low, or that the team explains what they are doing before they do it.
- Seeing Your Baby’s Birth: Ask if a clear or lowered drape is possible so you can see your baby being born.
- Immediate Connection: Request that your EKG leads are placed on your back to keep your chest free for immediate skin-to-skin contact with the baby if you are both stable. You can also ask for one of your arms to be left free of cuffs or IVs so you can touch your baby.
- Partner’s Role: Specify that you’d like your partner to announce the baby’s sex.
- Post-Operative Care: State your preference for the baby to stay with you and your partner in the recovery room, and for your partner to advocate for this to prevent unnecessary separation.
By having these preferences written down, your partner doesn’t have to guess what you would want. They have a clear, actionable list to work from, allowing them to be a confident and effective advocate on your behalf.
Why “Just Tell Me What to Do” Still Leaves All the Planning With You?
The phrase “just tell me what to do” is often said by partners with the best of intentions. It sounds helpful, willing, and supportive. However, it reveals a fundamental misunderstanding of what true support entails. This phrase keeps the birthing person in the role of project manager, still responsible for all the planning, thinking, and delegating. You are still carrying the entire cognitive load of the operation. You have to notice the need, formulate the task, and then direct your ‘helper’ to execute it—all while navigating the immense physical and mental demands of labour.
True partnership in labour, and indeed in parenting, involves a shift from task delegation to responsibility transfer. The goal isn’t for your partner to become an obedient assistant waiting for instructions. The goal is for them to become a co-owner of the experience, capable of anticipating needs, understanding the plan, and taking initiative. This article is your guide to achieving that transfer. It’s about briefing them so thoroughly that they understand the ‘why’ behind each preference, enabling them to think strategically on your behalf.
This is about more than just labour; it’s a foundational skill for co-parenting. As Dr. Rebecca Dekker of Evidence Based Birth® puts it, true advocacy is a learned skill that empowers the entire family unit. In the Evidence Based Birth Childbirth Class, the focus is clear: “We will teach you and your partner(s) how to be your own advocate—how to respectfully speak up for yourself, your partner, and your child. This is a skill you can use for the rest of your life!” When your partner moves beyond “just tell me what to do,” they are not just supporting you better in labour; they are stepping fully into their role as an equal parent and partner.
Key Takeaways
- True partner support is about transferring responsibility, not just delegating tasks, to avoid leaving the birthing person with the entire mental load.
- Practical, hands-on skills like counter-pressure and specific advocacy phrases for emergencies are teachable and build a partner’s confidence.
- Planning for the unexpected, such as a ‘Plan B’ for a C-section, empowers both partners and helps maintain a sense of control no matter how the birth unfolds.
Why Mothers Still Carry 71% of the Mental Load Even With “Hands-On” Partners?
The issue of briefing your birth partner is a microcosm of a much larger conversation: the unequal distribution of the mental load in parenthood. Even with partners who are “hands-on”—partners who change nappies, do night feeds, and are physically present—women often remain the default project managers of the family. They are the ones tracking appointments, researching sleep regressions, planning meals, and anticipating needs. This invisible, non-stop work of planning and organising is the mental load. It’s exhausting, and it often starts long before the baby arrives.
The statistic is stark and validating for many mothers. Research shows that women shoulder the majority of this cognitive labour. While the exact figure can vary, it is a significant and well-documented phenomenon that a mother’s mental workload increases dramatically postpartum. The title of this section refers to a commonly cited type of figure in this domain, where studies show mothers carry a disproportionate amount of the mental load. The request “just tell me what to do” during labour is the first sign of this dynamic taking root. It sets a precedent where the mother is the ‘knower’ and the partner is the ‘doer’, reinforcing a pattern that is difficult to break later on.
Therefore, the process of briefing your birth partner is your first and most powerful opportunity to actively co-create a different kind of partnership. This isn’t just about having a better birth experience; it’s about setting the foundation for a more equitable co-parenting journey. By teaching your partner not just what to do, but *how to think* about supporting you—how to anticipate needs, understand the underlying reasons for your preferences, and take initiative—you are offloading the mental load before it becomes cemented. You are training your co-pilot for the entire journey of parenthood, not just the takeoff. This strategic briefing is an investment in your future sanity and the long-term health of your partnership.
By intentionally and strategically preparing together, you are doing more than just planning for a single day. You are building the communication, trust, and shared responsibility that will serve your family for a lifetime. Start these conversations now, practice these skills together, and step into your birth experience as a truly united and empowered team.